Not all dental implant procedures are the same. Some patients need straightforward treatment that takes just one visit, while others face obstacles that require specialized skills and extra planning.
A complex implant case typically involves insufficient bone volume, gum disease, anatomical challenges like sinus cavities or nerve pathways, previous failed implants, or medical conditions that affect healing.
The difference between a routine implant and a complex one often determines which dentist you should choose. Experience matters significantly in challenging implant cases because these situations require advanced techniques, precise planning, and the ability to adapt when unexpected issues arise.
A dentist who regularly handles difficult cases brings problem-solving skills that go beyond basic implant placement.
Understanding what makes your case complex helps you ask the right questions and find a provider with the right background. Whether you’re dealing with bone loss, multiple missing teeth, or have been told you’re not a candidate for implants, knowing the challenges involved can guide you toward better treatment options.
Key Takeaways
- Complex implant cases involve bone loss, gum disease, anatomical obstacles, or failed previous treatments that require specialized techniques
- Experienced implant specialists can combine advanced methods like bone grafting, angled implants, and 3D imaging to solve difficult cases
- Proper evaluation with detailed imaging and treatment planning improves success rates even in challenging situations
Book a complex implant evaluation in Munster and Schererville, IN to explore advanced options like bone grafting and full arch implants.
Defining a Complex Implant Case
A complex dental implant case goes beyond basic implant placement and requires specialized planning, advanced techniques, or additional procedures to achieve success. Multiple factors can transform a straightforward implant procedure into one that demands expertise in implantology and careful consideration of your unique anatomical or medical situation.
Key Differences from Simple Implant Cases
Simple implant cases typically involve replacing a single tooth in healthy bone with adequate volume and density. Your gums are healthy, you have no medical conditions affecting healing, and the implant placement follows standard protocols.
Complex implant cases require you to work with a specialist who can handle challenges beyond routine procedures. The doctor must determine whether implants are the best option within a framework of a partially or fully edentulous jaw. Hard and soft tissue foundations may be inadequate for implant placement and need augmentation before placing fixtures.
Your treatment timeline extends significantly. While simple cases might take three to six months from start to finish, complex cases can require staged procedures over longer periods to ensure proper osseointegration and tissue healing.
Common Factors That Increase Complexity
Several conditions transform your implant case into a complex one requiring specialized attention:
Insufficient bone volume or quality tops the list of complications. Years of tooth loss cause your jawbone to shrink through resorption, leaving inadequate support for standard dental implants.
Severe gum disease creates an environment where bacteria threaten implant success. Your periodontal tissues need treatment before implant placement can proceed safely.
Anatomical challenges include proximity to sinus cavities in your upper jaw or nerve pathways in your lower jaw. These structures require careful navigation during surgery.
Previous failed implants leave you with compromised bone and tissue that needs regeneration. Medical considerations like diabetes or medications can affect healing and osseointegration.
Multiple missing teeth with bite issues require comprehensive planning. Your restorations must restore proper function while addressing alignment problems.
Case Examples of Varying Difficulty
Understanding real scenarios helps you recognize where your situation falls on the complexity spectrum.
A simple case involves you losing a single molar with healthy surrounding teeth and bone. The implant placement takes one appointment, and you receive your final restoration after healing completes in three to four months.
A moderate case might involve you needing three implants in your lower jaw with minor bone grafting at one site. Your treatment requires two surgical appointments and five to six months total time.
A complex case includes you wearing dentures for years with severe bone loss requiring zygomatic implants or extensive grafting procedures. Treatment planning complex implant cases demands thorough evaluation of your medical history, proper dental diagnosis, and appropriate planning.
Your full-mouth reconstruction might need multiple surgeries staged over twelve months or more to achieve stable, functional restorations.
Need solutions for complex dental implant cases in Schererville and Munster, IN? Schedule a surgical consult and get a clear plan.
Anatomical and Structural Challenges
The physical structure of your jaw and surrounding tissues plays a major role in determining how difficult an implant procedure will be. Problems with bone quantity, proximity to vital structures, and variations in anatomy can turn what seems like a straightforward case into one requiring specialized expertise.
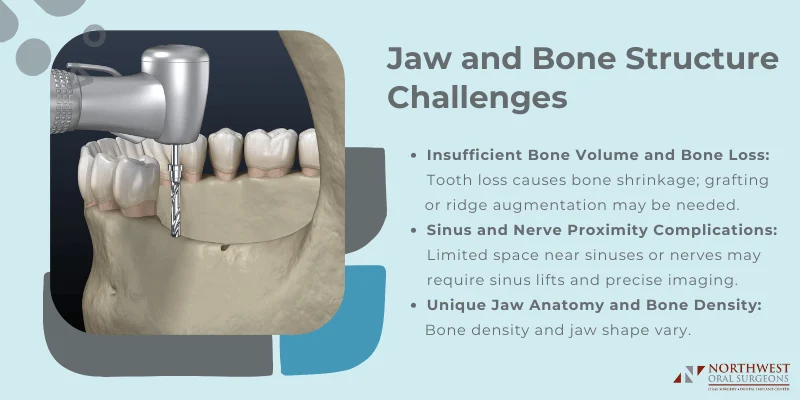
Insufficient Bone Volume and Bone Loss
Your jawbone needs adequate height, width, and density to support a dental implant. When you lose a tooth, the surrounding bone begins to deteriorate over time. This bone loss can leave you without enough bone volume to place an implant safely.
Anatomical challenges like insufficient bone volume require additional procedures before implant placement. Your dentist may recommend bone grafting to rebuild lost bone structure. Ridge augmentation can widen or heighten the jawbone in areas where it has shrunk.
In severe cases, traditional implants may not be possible even with grafting. Alternative solutions include zygomatic implants that anchor into your cheekbone rather than the jaw. Tilted implants can also bypass areas with poor bone quality by angling through stronger bone sections.
Sinus and Nerve Proximity Complications
The upper back jaw sits very close to your sinus cavities. The lower jaw contains important nerves that control sensation in your lips, chin, and tongue. Placing implants too close to these structures can cause serious complications.
When placing implants near the sinus, your dentist must carefully measure available space. A sinus lift procedure raises the sinus floor and adds bone underneath to create more room. This allows for proper implant length without penetrating the sinus cavity.
Nerve proximity requires precise planning using advanced imaging. Your dentist must map the exact path of nerves to avoid damaging them during placement. Even a few millimeters can make the difference between a successful procedure and nerve injury.
Unique Jaw Anatomy and Bone Density
No two patients have identical jaw structures. Your bone density can vary significantly from one area of your mouth to another. Some people naturally have thinner or more porous bone that makes implant stability harder to achieve.
Cases with complex anatomical structures benefit from computerized navigation systems during surgery. These tools help your dentist place implants with precision despite unusual anatomy. Areas with low bone density may require longer healing times or specialized implant designs that distribute forces differently.
Previous dental work, injuries, or medical conditions can also change your jaw structure in unexpected ways. Your dentist needs experience reading scans and adapting treatment plans to work with your specific anatomy rather than against it.
Get answers for complex dental implant cases. Request a specialist consultation and a personalized treatment roadmap.
Advanced Surgical and Restorative Techniques
Complex implant cases demand specialized procedures that go beyond basic implant placement. These techniques address bone deficiencies, anatomical limitations, and the need for extensive restorations while managing potential complications.
Bone Grafting and Bone Augmentation
When you don’t have enough bone to support an implant, bone grafting becomes necessary. In one clinical study, 50.3% of patients required a bone graft during implant surgery.
Your dentist may use different materials including your own bone, processed human bone, or xenograft from animal sources.
Bone augmentation procedures can add width or height to your jaw. One approach uses bone blocks harvested from another area of your mouth and fixed to the deficient site with tiny screws.
The bone block technique carries higher risk compared to other methods. However, when successful, it can create significant bone volume in areas where implant placement would otherwise be impossible.
Some cases allow dentists to work around bone limitations entirely. By carefully positioning implants in available bone between nerves and other structures, you might avoid grafting altogether.
Sinus Lifts and Guided Bone Regeneration
Your upper back teeth sit near your sinuses, which often limits bone height. A sinus lift raises the sinus floor and adds bone material underneath to create space for implants.
Guided bone regeneration uses special membranes to protect grafted bone while it heals. These membranes come in different types including collagen, Teflon, and titanium, each with specific benefits.
Your dentist prepares the recipient site by removing surface layers and creating small holes in the cortical bone. This controlled trauma releases growth factors that help new bone form.
Healing caps may be placed immediately if your implants achieve enough initial stability. Otherwise, your dentist will use plugs and wait for the bone to integrate before adding the healing components.
Full-Arch and All-on-4 Restorations
Full-arch restorations replace all teeth in your upper or lower jaw using multiple implants. These differ dramatically from single-tooth implant procedures in planning and execution.
The All-on-4 technique uses four strategically angled implants to support an entire arch. This approach often eliminates the need for bone grafting by positioning implants where bone naturally exists.
You might receive different prosthesis types depending on your situation. Options include fixed horseshoe-shaped restorations for your upper jaw or implant-supported denture designs secured to a bar framework.
Multiple implants require precise angulation and spacing. Your dentist must ensure adequate distance between implants so bone tissue receives proper nutrition and heals correctly.
Soft Tissue Management and Complications
Soft tissue complications can occur even when bone integration succeeds. Poor tissue health around your implants may lead to infection or aesthetic problems.
Your dentist manages soft tissues through careful suturing techniques and proper implant depth. Placing implants slightly below bone level creates space for healthy gum attachment and an attractive appearance.
Common soft tissue issues include:
- Inadequate attached gum tissue around the implant
- Inflammation from trapped food or bacteria
- Recession exposing implant threads
- Poor pink tissue aesthetics in visible areas
Platelet-rich plasma from your own blood can be placed around implants to promote healing. This material helps fill voids and supports soft tissue regeneration during recovery.
The aesthetic zone presents unique challenges. Your front teeth require not just functional restoration but also natural-looking gum contours that match your smile.
Role of Diagnostics and Treatment Planning
Proper diagnostics and planning form the foundation of successful complex implant procedures. Advanced imaging tools and digital planning software help identify potential problems before surgery begins, while surgical guides ensure precise implant placement during the procedure.
Comprehensive Evaluation and 3D Imaging
Your dentist needs a complete picture of your oral health before placing implants in complex cases. This starts with a thorough evaluation of your medical history and a detailed clinical examination of your mouth.
Advanced imaging plays a critical role in this process. CBCT scans provide three-dimensional views of your jaw bone, showing bone density, nerve locations, and sinus positions. These scans reveal anatomical challenges that regular X-rays might miss.
Comprehensive evaluation and 3D imaging help your dental team measure bone volume and assess whether you need additional procedures like bone grafting.
Panoramic X-rays and intra-oral scans add more information to create a complete diagnostic picture. This data collection ensures your treatment team understands exactly what they’re working with before they begin.
Treatment Planning with Digital Tools
Digital planning software transforms raw diagnostic data into actionable treatment plans. These programs let your dentist visualize treatment outcomes before any dental work begins, which is especially valuable for complex cases involving multiple implants or full-arch restorations.
Computer-aided design (CAD) software creates a virtual version of you as a patient. Your dental team can use this digital model to plan implant positions, test different approaches, and predict how each decision affects the final result.
This technology helps identify specific needs early in the process. Your dentist might discover you need crown lengthening or orthodontic adjustments before implant placement.
Digital planning also improves communication between different specialists working on your case, ensuring everyone follows the same treatment roadmap.
Use of Surgical Guides and Guided Surgery
Surgical guides translate digital plans into physical reality during your procedure. These custom-made templates fit over your teeth or gums and contain precise holes that direct drill placement during surgery.
Guided implant surgery offers significant advantages in complex cases with anatomical challenges. The guides ensure implants go exactly where planned, avoiding nerves and sinuses while achieving optimal angles for your final restoration.
This precision becomes especially important when placing multiple implants or working with limited bone. Guided surgery reduces the risk of improper positioning that could turn a planned fixed prosthesis into a removable appliance. The technique also typically results in less surgical time and more predictable healing for you as the patient.
Importance of Specialist Experience and Multidisciplinary Collaboration
Complex implant cases require dentists with specialized training and often benefit from a team-based approach. The right combination of expertise ensures better outcomes and fewer complications for patients with challenging dental situations.
Specialized Implant Training and Credentials
Not all dentists receive the same level of implant training during dental school. Basic programs may cover single-tooth replacements, but advanced implant training teaches techniques for full-arch restorations, bone grafting, and implant placement in compromised bone.
Organizations like the American Academy of Implant Dentistry offer comprehensive implant training through continuing education courses and fellowship programs. Dentists who pursue these credentials gain hands-on experience with complex surgical protocols and prosthetic workflows.
Look for providers who have completed residencies in implant dentistry or earned designations such as Associate Fellow or Fellow from professional implant organizations. These credentials indicate hundreds of hours of additional education beyond dental school.
Some dentists also attend specialized programs through institutions like High Tech Dental Seminars to stay current with digital planning tools and guided surgery techniques.
When to Consult a Prosthodontist, Periodontist, or Oral Surgeon
Your general dentist may refer you to specialists depending on your case complexity. A prosthodontist specializes in designing and fabricating complex restorations, including multi-unit implant bridges and full-mouth rehabilitations. They excel at treatment planning when multiple teeth need replacement.
A periodontist focuses on gum health and the bone that supports implants. They handle cases requiring bone grafting, sinus lifts, or soft tissue management around implants.
An oral surgeon performs complex extractions and places implants in challenging anatomical situations, such as near nerves or in areas with severe bone loss.
Some cases benefit from an orthodontist who can create proper spacing before implant placement. An implantologist is a dentist with focused training specifically in implant procedures, though this isn’t always a formal specialty designation.
Multidisciplinary Team Approach for Complex Cases
Interdisciplinary collaboration is essential for managing complex dental cases that involve multiple treatment phases. When your case requires extensive work, specialists coordinate their efforts to create a unified treatment plan that addresses all your needs.
For example, a periodontist might perform bone grafting first, then an oral surgeon places the implants, and finally a prosthodontist designs your final restoration. An implant specialist plays a key role in addressing these concerns, offering comprehensive expertise tailored to each step of the process.
This team-based approach is particularly valuable for full-mouth reconstructions or cases involving medical conditions that affect healing. Digital communication tools allow your specialists to share scans, X-rays, and treatment plans seamlessly.
Patient Considerations and Factors Affecting Outcomes
Your overall health, dental history, and daily habits play major roles in whether your dental implant procedure will succeed. These personal factors can add complexity to your case and require your dentist to adjust the treatment approach.
Medical Conditions and Systemic Risk Factors
Certain health conditions make implant surgery more challenging and can affect how well your implants heal. Diabetes slows down wound healing and can reduce implant stability if your blood sugar isn’t well controlled. If you smoke, your risk of implant failure increases because tobacco restricts blood flow to your gums and jawbone.
Osteoporosis weakens your bone density, which affects how well implants integrate with your jaw. Some medications for osteoporosis can also cause problems with bone healing. If you take blood thinners, your dentist needs to coordinate with your doctor to manage bleeding risks during surgery.
Autoimmune diseases like rheumatoid arthritis or lupus can interfere with implant integration. Radiation therapy to your head or neck area damages bone cells and makes it harder for implants to take hold. Your dentist must evaluate these medical problems and resulting compromises in treatment before planning your procedure.
Previous Dental Work and Implant Failures
Your past dental treatments tell an important story about what to expect. If you’ve had a previous implant failure, your dentist needs to understand why it happened before placing a new one. Failed implants often leave behind damaged bone that requires grafting.
Large posts and cores from old root canals can complicate tooth extraction and implant placement. Your dentist must decide whether to remove these structures or work around them. Previous gum disease might have destroyed the bone around your teeth, leaving less support for new implants.
Multiple missing teeth create additional challenges because your dentist must plan for proper spacing and support. If you’ve had bridges or dentures for years, your jawbone may have shrunk from lack of use. This bone loss affects implant stability and might require bone grafting before you can receive implants.
Treatment Timeline and Patient Communication
Your treatment timeline depends on how much preparation work you need before implant surgery. Simple cases might take three to six months from start to finish. Complex cases requiring bone grafts or multiple tooth extractions can take a year or longer.
After tooth extraction, you typically wait three to six months for the bone to heal before implant placement. The implant then needs another three to six months to fuse with your jawbone. Your dentist should explain these waiting periods upfront so you understand the full commitment.
Clear communication prevents frustration during the long treatment process. Your dentist should discuss any issues they discover before starting work, not after. When problems come up later, it can look like an excuse rather than a proper diagnosis.
Oral Hygiene and Maintenance After Surgery
Your daily cleaning habits directly impact whether your implants last. Poor oral hygiene is one of the top reasons for implant failure after surgery. Bacteria buildup around implants causes inflammation that destroys the surrounding bone.
You need to brush twice daily and floss around your implants just like natural teeth. Special interdental brushes help clean hard-to-reach areas. Regular dental checkups let your dentist catch problems early before they threaten your implants.
Your chewing function affects implant stability, especially if you grind your teeth at night. A night guard protects your implants from excessive force. Following your dentist’s aftercare instructions during healing is critical for successful implant integration and long-term tooth replacement success.
Frequently Asked Questions
Several factors can turn a straightforward implant into a challenging procedure, from your overall health to the quality of your jawbone. Understanding these elements helps you know what to expect during treatment.
How do patient medical conditions affect dental implant complexity?
Your overall health plays a big role in how complicated your implant procedure might be.
Conditions like diabetes can slow down healing and make it harder for the implant to fuse with your jawbone.
If you have an autoimmune disease, your body might not respond to the implant the way it normally would.
Heart disease and blood pressure issues can also add extra steps to your treatment plan.
Your dentist needs to know about all your medical conditions before starting. This information helps them plan the right approach for your specific situation.
What factors determine the difficulty of a dental implant procedure?
The number of teeth you need to replace makes a big difference in how complex your implant case becomes.
Replacing one tooth is usually straightforward, but restoring multiple teeth or a full arch requires more planning.
The condition of your jawbone matters a lot too. If you’ve been missing teeth for a long time, your bone may have started to break down.
Multiple implants, angled placement, or anatomical challenges all add to the difficulty level. Your mouth’s unique structure can present obstacles that need special attention.
Can bone density influence the success rate of implants?
Your jawbone density directly affects whether an implant will hold in place properly. Natural tooth roots keep your jawbone healthy by stimulating it, but when teeth go missing, that stimulation stops.
Without enough bone density, your jaw can’t provide the strong foundation an implant needs. This doesn’t mean you can’t get implants, though.
A bone graft can add healthy bone tissue to strengthen your jaw first. This common procedure helps create the support needed for successful implant placement.
Why is experience important for handling complicated implant cases?
The difference between success and failure often comes down to your surgeon’s experience and problem-solving skills. An experienced dentist has seen many different situations and knows how to handle unexpected challenges.
Complex cases need someone who can adapt their approach when things don’t go as planned. Your dentist’s years of practice help them spot potential problems before they happen.
They also know the best techniques for working around anatomical challenges. This expertise can mean the difference between a successful implant and one that fails.
How does the location of the implant placement impact the complexity of the surgery?
Some areas of your mouth are harder to work with than others. Back teeth often need more bone support because they handle more chewing force.
The upper jaw can be trickier because the bone is usually softer than in the lower jaw. Areas near sinuses or nerves require extra care and precision.
Front teeth present their own challenges because the results need to look natural. Your dentist has to think about both function and appearance in these visible areas.
What are the common challenges faced during complex dental implant surgeries?
Limited bone support creates one of the biggest obstacles in implant surgery. Your dentist needs to work with what’s available or build up the area first.
If you grind your teeth at night, the extra pressure can lead to bone loss around implants. A protective mouthguard can help prevent this problem.
Tobacco use dramatically increases the risk of implant failure. Nicotine restricts blood flow to your mouth, which can stop the implant from bonding with your jawbone properly.




